Part 1: What is Hashimoto’s and How Is It Diagnosed?
One of the conditions we see with increasing frequency at our office is Hashimoto’s disease, also known as Hashimoto’s thyroiditis. Hashimoto’s is an autoimmune condition that is the leading cause of hypothyroidism (underactive thyroid function).
To help you better navigate this complex condition, I am launching a three-part blog series to address common questions and misconceptions:
- Part 1: Defining Hashimoto’s and the testing required for an accurate diagnosis.
- Part 2: Exploring the “root cause” mechanisms—how and why Hashimoto’s develops.
- Part 3: An integrative, patient-focused approach to treatment and recovery.
The Anatomy of an Attack
As an autoimmune condition, Hashimoto’s occurs when the immune system mistakenly identifies healthy thyroid tissue as a foreign invader. It mounts an immune response that leads to the progressive destruction of thyroid cells.
As more tissue is damaged over time, the brain attempts to compensate. The pituitary gland releases increased amounts of Thyroid Stimulating Hormone (TSH) to “shout” at the thyroid to work harder. An elevated TSH is often the first “smoke detector” indicating that thyroid function is altered and warrants further investigation. If the underlying autoimmunity isn’t addressed, the brain eventually cannot release enough TSH to maintain normal function, and the patient begins to suffer.
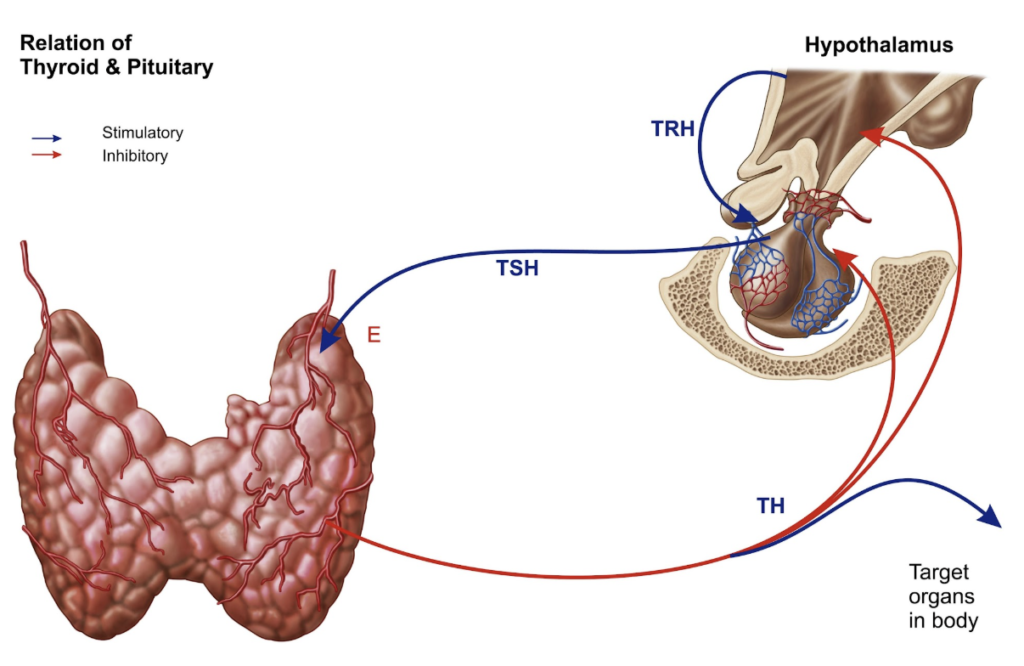
Understanding the “Master Switch”
In a healthy body, the thyroid uses iodine to produce T4 (the storage form of the hormone). T4 is then converted in various tissues into Free T3—the bioactive “master metabolic switch.” T3 controls critical functions including:
- Heat regulation and body temperature
- Heart rate
- Mental cognition and mood
- Gut motility and digestion
When T3 levels drop (hypothyroidism), the body slows down. Patients often experience fatigue, sluggishness, cold intolerance, weight gain, thinning hair (specifically the outer third of the eyebrows), constipation, brain fog, and depression.
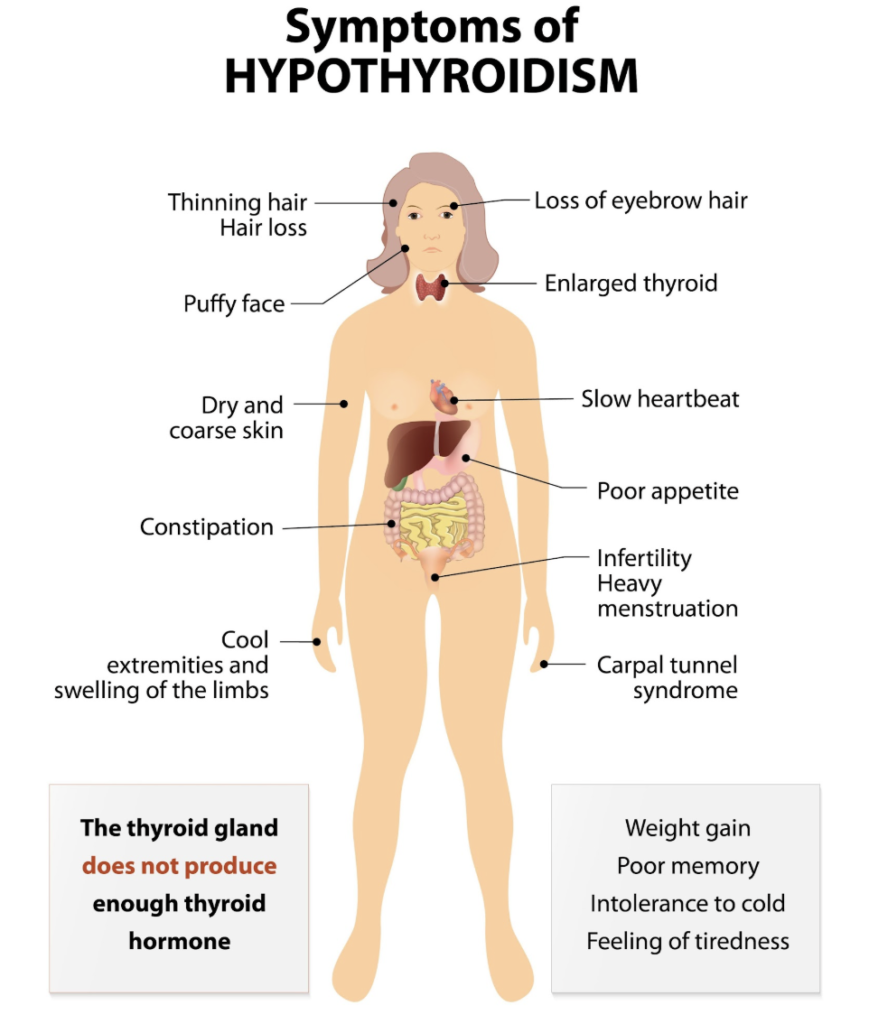
How We Make a Diagnosis
To properly diagnose Hashimoto’s, we cannot rely on TSH alone. We must see an elevation in specific thyroid antibodies via a comprehensive blood panel:
- TPO Antibodies (Thyroid Peroxidase): TPO is the enzyme that converts dietary iodine into a usable form for hormone production. Approximately 90-95% of Hashimoto’s patients test positive for these.
- TG Antibodies (Thyroglobulin): Thyroglobulin is a protein that helps synthesize and store thyroid hormones. About 60-80% of patients test positive for these.
If you test positive for either, it confirms an active autoimmune attack against your own thyroid gland. The extent of the damage depends largely on how long the attack has gone untreated.
Clinical Pearl: Autoimmunity rarely travels alone. Patients with one autoimmune disease are significantly more susceptible to developing others. If you test positive for thyroid antibodies, it is vital that your doctor performs comprehensive testing to rule out other underlying autoimmune conditions.
Summary
Hashimoto’s is a progressive condition where the immune system mistakenly destroys healthy thyroid cells, eventually leading to the systemic symptoms of hypothyroidism.
In Part 2, we will dive into the “Why”—how Hashimoto’s starts and the steps you can take to prevent or slow its progression.
Post written by Dr. Riley Kulm, DC. Check out his bio here.

